All kids have meltdowns. It’s a part of life. And it’s a HUUUUGE part of SpEd life.
Which means that, as professionals dealing with difficult situations, we are all familiar with that one classic question:
Is it a sensory need or behavioral?


Well, let’s start with what we already know.
Children with autism often have challenges with sensory processing.
These can lead to “meltdowns” caused by sensory overload.
Now partner that with the fact that these students can also have difficulties expressing their needs and wants - - - which can lead to behavioral issues or “tantrums”.
It’s no wonder that this dilemma can leave even the best of us scratching our heads.
So how the heck do we know the difference? And how are we going to approach the situation once we’ve figured it out?
First, take solace in the idea that you are NOT alone.

This is a challenge for many people, including SpEd pros who have been in the game for years.
In order to sort this out, let’s go back to the good ‘ole school days and start with some basic definitions.
A sensory “meltdown” is caused by a child feeling overwhelmed by incoming sensory input.
Children with normal sensory processing can take in various sensations simultaneously, process it and form a response. And they are doing it literally every second of the school day.
However, for our friends that have sensory processing difficulties, processing various sensations can be incredibly hard and overwhelming. The school environment can be a recipe for sensory overload.
For example, picture a child on the playground. The experience might look something like this:
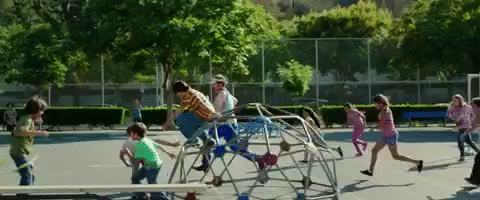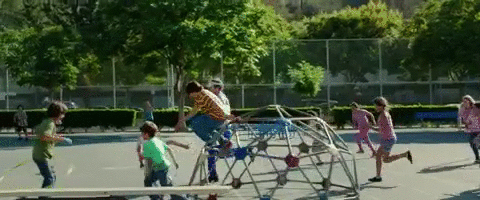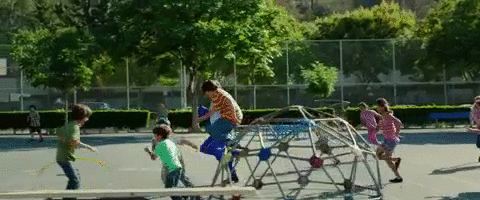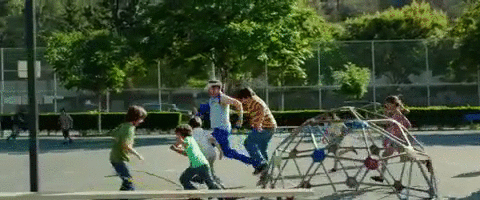
Visual stimuli: Children running, cars passing, balls rolling every which way . . . and don’t forget the birds and squirrels.
Auditory stimuli: Children laughing & yelling (LOTS of yelling), lawn mowers, and whistles blowing (what did that whistle mean, again?)
Tactile stimuli: Physical contact during games or even accidentally getting touched or pushed by a peer.
It’s a LOT to deal with.
And it’s all happening at the same time.
If a child becomes too bombarded with sensory input, they generally go into a “flight or fight” response.
This is a physical response that the student is NOT in control of. It can often look like a “meltdown.” You might see crying, refusal to follow directions, running away or even hitting or kicking.
A “tantrum,” on the other hand, is fueled by behavior (and not sensory overload).

Behaviors occur for a variety of reasons.
These reasons may include difficulty communicating a need, issues with impulsivity or other attention deficits, or a lack of emotional self-regulation.
Okay, so we’ve got some definitions down. What’s next?
How about some tips on how to identify a sensory meltdown from a tantrum?
No need to scream “YES!!!” We can’t actually hear you ;)
If it’s a sensory need:
- Look for signs such as a red or pale face, withdrawal from the group or activity, an increase in self-stimming, rigidity or sweating.
- The meltdown does not stop immediately after the need is met or situation is changed. The fight or flight reaction takes time to dissipate.
- Notice if proactive methods (such as giving breaks at the first sign of distress) prevent further escalation.
If it’s a behavioral concern:
- The tantrum stops once the student gets their wants met.
- Preventative measures, such as giving breaks, may not be successful. The student is focused on getting their demand met.
Although “tantrums” and “meltdowns” may appear similar, the causes are very different and need to be approached accordingly.
There are many ways to support students with behavioral needs. And it varies wildly from classroom to classroom & from student to student.
At AdaptEd we rely on the support of our behaviorists, so we are going to refer you there.
However, we’ve got a great OT response to sensory meltdowns for you. (We know, this is what you have been waiting for!)
What to do for a sensory meltdown:
It’s important to remember that the child is now in a “fight or flight” state. They need to be brought back to a calm, safe place.
- Limit verbal directions, use gestures as much as possible
- Provide an alternate space such as a quiet corner or sensory room where there is limited stimulation
- Provide strategies for them to utilize (noise cancelling headphones . . . hand fidgets)
- Ask them what they need and provide visuals for options, such as a shoulder squeeze or walk
- Try to prevent the child from reaching future “meltdown” states by anticipating overwhelming environments. The child may exhibit escalation behaviors that can cue you in.
The bottom line is that we don’t have a magical recipe for knowing if it is sensory or behavioral (Sorry!!!).
It can be extremely difficult to tease out. So be sure to consult your occupational therapist and behaviorist.
We ALWAYS advocate for the team approach to all circumstances. The students benefit most when we all put our areas of expertise together and solve the puzzle!

Plus, let’s be real here- using the people around us as resources only makes life easier. And we could all use a little bit of EASY now and then.
XOXO,
Vanessa, AdaptEd OT
P.S. In case you DO pinpoint a sensory need in your student, you may want to check out some of our handy sensory resources! Made by an OT (Me!!!!!)




